Understanding the Metabolic Link Between Erythropoiesis and Iron Bioavailability
09 Mar, 2026
3836 Views 0 Like(s)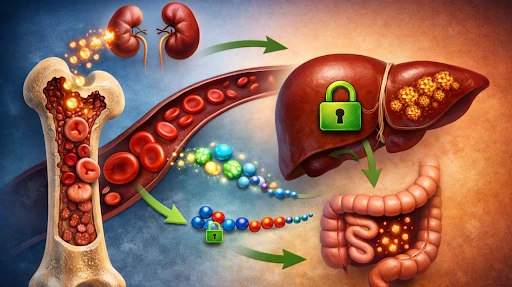
The bone marrow produces red blood cells (erythropoiesis), which requires a lot of iron. While the human body gets iron from the diet, the liver produces hepcidin, a hormone that controls iron levels. How does bone marrow tell the liver to release more iron?
The communication between bone marrow and liver remained a mystery for decades. It was in 2014 that scientists finally identified the primary messenger linking blood production to iron supply: a hormone called erythroferrone, or ERFE.
How the Erfe Circuit Works
The human body relies on a very specific pathway to ensure the required availability of iron for the production of new blood cells.
-
The kidneys release a hormone called erythropoietin (EPO) in response to low oxygen in the blood.
-
EPO travels to the bone marrow and stimulates erythroblast production (the production of young red blood cells). These cells secrete erythroferrone into the blood.
-
Erythroferrone travels to the liver and tells it to stop the secretion of hepcidin.
When hepcidin is low, the body absorbs more iron from food and releases stored iron from the liver and spleen. This ensures that bone marrow receives a steady supply of iron to produce hemoglobin.
How Erfe Blocks the Signal
The liver produces hepcidin when it receives a signal from proteins called Bone Morphogenetic Proteins (BMPs). Erythroferrone does not reach the liver; it works as an inhibitor instead, trapping the BMP protein in the blood. As the BMP signal never reaches the liver, the SMAD signaling pathway in the liver is not activated. This pathway is the internal switch for the HAMP (hepcidin) gene.
Erfe in Chronic Disease: β-thalassemia
Erythroferrone levels stay low in a healthy body unless there is an emergency. However, certain diseases, such as β-thalassemia, break this system. The bone marrow becomes hyperactive in β-thalassemia, constantly trying to make red blood cells. However, due to a genetic defect (a mutation in the HBB gene causing β-thalassemia), these cells die before they mature.
As a result, the marrow never stops secreting erythroferrone, leading to iron overload. Over time, iron buildup can cause permanent damage to the heart and liver.
Clinical Applications
Using Erfe as a Biomarker
It is hard to tell if a patient’s iron levels are low due to a lack of iron or inflammation. Quantification of Erfe allows doctors to measure the pressure on the bone marrow. High Erfe indicates that the marrow is demanding more iron. This helps doctors determine the dosage of EPO or iron for a patient suffering from chronic kidney disease (CKD).
Erfe as a Drug Target
Blocking Erfe could be a treatment when too much Erfe leads to iron overload. Scientists are currently developing Erfe-neutralizing antibodies, engineered to naturally developed proteins that bind to the N-terminal domain of the hormone erythroferrone, preventing suppression of hepcidin.
This helps the body naturally block iron absorption, which could reduce the need for harsh "chelation" drugs that are currently used to strip iron from the body.
New Areas of Study
New research suggests that erythroferrone might be produced in other places, such as skeletal muscle. This suggests that the hormone might help the body manage iron during intense physical exercise. Researchers are also studying the interaction between Erfe and inflammation. It is well understood that inflammation raises hepcidin, and Erfe lowers it. The scientific community is trying to figure out which signal wins when a patient is both sick and anemic.
Ongoing studies aim to refine erythroferrone-based diagnostics and therapies, potentially improving personalized treatment strategies for anemia, iron overload disorders, and other hematologic and metabolic conditions worldwide.
Researchers rely on human erythroferrone (ERFE) ELISA kits to detect and quantify erythroferrone in a sample. AAA Biotech is the leading supplier of a wide range of kits for immunoassays.
Comments
Login to Comment