Back pain can change almost everything, from the way you work and sleep to how confidently you move through your day. For many people, one of the hidden causes of ongoing back pain is Spondylolisthesis, a spinal condition that happens when one vertebra slips forward over the one below it. This movement can create instability in the spine, irritate nearby nerves, and lead to pain, numbness, or weakness.
While many cases can improve with physical therapy, medications, or injections, some patients eventually need surgery. Today, one of the most effective options is minimally invasive spine surgery, often called MISS. This advanced approach can stabilize the spine while reducing tissue damage and shortening recovery time.
At Atlantic Brain and Spine, specialists use advanced minimally invasive techniques to help patients with complex spine conditions, including spondylolisthesis.
What Is Spondylolisthesis?
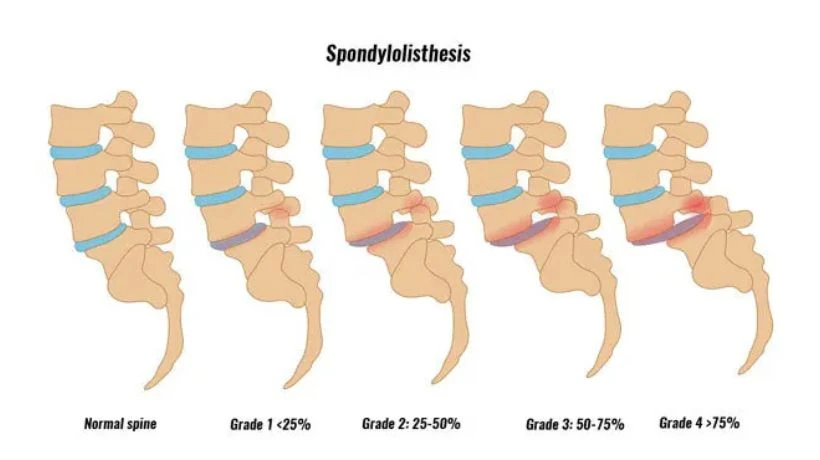
Spondylolisthesis occurs when a vertebra moves out of its normal position. This can happen for several reasons, including age related wear and tear, stress fractures, trauma, or congenital spinal changes.
Common symptoms may include:
- Persistent lower back pain
- Tightness in the hamstrings
- Pain that travels into the legs
- Tingling or numbness
- Weakness while walking or standing
- Reduced flexibility or balance
In more advanced cases, the slipped vertebra may compress nearby nerves, making everyday activities more difficult.
When Is Surgery Needed?
Not every patient with spondylolisthesis needs surgery. Doctors usually begin with conservative treatment such as physical therapy, anti inflammatory medications, activity modification, or spinal injections.
Surgery may be recommended when:
- Pain continues despite non surgical treatment
- Nerve symptoms are getting worse
- Walking or standing becomes difficult
- Spinal instability is affecting daily life
- Imaging shows significant vertebral slippage
The goal of surgery is to relieve pressure on nerves, restore spinal stability, and improve quality of life.
What Is Minimally Invasive Spine Surgery?
Minimally Invasive Spine Surgery is a modern surgical approach that allows spine surgeons to treat spinal problems using smaller incisions and specialized tools.
Instead of separating large sections of muscle like in traditional open surgery, surgeons work through narrow pathways using advanced imaging, microscopes, or robotic guidance. This allows them to reach the affected area with greater precision and less disruption to surrounding tissue.
How Minimally Invasive Surgery Helps Treat Spondylolisthesis
Depending on the severity of the condition, minimally invasive surgery may involve decompression, spinal fusion, or both.
1. Relieves Pressure on Nerves
If the slipped vertebra is compressing spinal nerves, surgeons can remove the tissue or bone causing the pressure. This often helps reduce leg pain, numbness, and weakness.
2. Stabilizes the Spine
In cases of instability, spinal fusion may be performed. During this procedure, the affected vertebrae are secured using screws, rods, or implants to restore alignment and prevent further movement.
3. Protects Healthy Muscle and Tissue
Because the incisions are smaller, there is less damage to muscles and soft tissues. This can lead to less postoperative discomfort and improved mobility during recovery.
4. Supports Faster Recovery
Many patients experience shorter hospital stays, lower blood loss, and a quicker return to normal activities compared with traditional open surgery. Some procedures may even be performed on an outpatient basis.
Benefits of Minimally Invasive Spine Surgery
Patients often choose minimally invasive techniques because of the potential benefits:
- Smaller incisions
- Less blood loss
- Lower infection risk
- Reduced postoperative pain
- Less visible scarring
- Faster rehabilitation
- Earlier return to work or daily activities
Every patient is different, so the best surgical plan depends on your symptoms, spinal imaging, and overall health.
Is Minimally Invasive Surgery Right for You?
Minimally invasive surgery can be highly effective for many people with spondylolisthesis, but not every case is the same. A complete evaluation by an experienced spine specialist is essential to determine the safest and most effective treatment approach.
If back pain, leg pain, or spinal instability is affecting your life, speaking with a spine expert can help you understand your options and make a confident decision.
Conclusion
Spondylolisthesis can make simple daily activities feel challenging, but treatment options have come a long way. Minimally invasive spine surgery offers a modern, effective way to reduce pain, restore stability, and help patients return to the activities they enjoy.
With smaller incisions, advanced technology, and faster recovery times, this approach is changing the way spinal conditions are treated.
Frequently Asked Questions
1. Can spondylolisthesis heal without surgery?
Mild cases often improve with physical therapy, medication, and lifestyle changes. Surgery is usually considered when symptoms continue or nerve compression worsens.
2. Is minimally invasive spine surgery painful?
Most patients experience less postoperative pain compared with traditional open surgery because there is less muscle disruption.
3. How long does recovery take after minimally invasive spine surgery?
Recovery varies by procedure and patient health, but many patients return to light activities within a few weeks.
4. Is spinal fusion always needed for spondylolisthesis?
Not always. Some patients only need decompression, while others benefit from fusion to restore spinal stability.
5. Who is a good candidate for minimally invasive spine surgery?
Candidates usually include patients with persistent pain, nerve compression, or spinal instability that has not improved with conservative treatment.

Comments
Login to Comment